Spider Veins:
Causes, Symptoms,
and Treatment.
What Is the Definition of Spider Veins?
Do you have thin, spindly veins that resemble spider legs or spider webs on your legs? These common telangiectasias are known as spider veins for their appearance. Red, blue, or purple, they often present in clusters at the outer layer of skin between the dermis and epidermis, which is why you can see them. While they aren’t always symptomatic, they aren’t healthy either, often stemming from an issue called chronic venous insufficiency.
Why Do Spider Veins Develop?
If you live long enough, you’ll probably develop a spider vein or two. Over half of Americans, (more women than men) have these damaged veins that are visible under the skin. The veins in your legs have a crucial task: transporting deoxygenated blood back to the heart, where it’s then routed to the lungs to collect oxygen. Once oxygenated, blood travels south from the lungs through the arteries, which return it to the veins to repeat the process. Deep veins do the heavy lifting, but the veins near the surface of your skin (saphenous) also share the task. These veins depend on valves to close once blood passes through them, so that blood arrives at the heart, rather than flowing back down to your feet.
When the valves don’t close tightly, blood collects, creating pressure on the vein walls. That pressure causes new dead-end veins to branch out from the overburdened vein. Those tiny spider veins spreading across your leg don’t take the blood where it needs to go. This taxes your leg veins as they work harder to do their job (chronic venous insufficiency). As a result of this impaired circulation, patients might feel heaviness or fatigue in their legs. They might deal with cramping, restless sensations, swelling, or pain upon contact. Other patients have no symptoms to speak of. Most notice their symptoms are worse with prolonged sitting or standing and better when they’re active.
Are You at Risk for Spider Veins?
Spider veins are common in all adults, especially women, particularly after turning 30. If both of your parents had spider veins, you’ll almost certainly develop them too. Elevated estrogen increases spider vein formation, so pregnant women and those using birth control or hormone therapy are extra susceptible. But injury to the skin’s surface or sun damage can also cause spider veins, as can sitting or standing too long on the job. Hairdressers, teachers, drivers, pilots, and healthcare workers are common patients at Long Island Vein Centers.
Do Spider Veins Cause Symptoms?
Many people don’t have any spider vein symptoms, other than mild stinging or burning sensations when they form. The majority of patients seek treatment because they’re unhappy with how spider veins look. But the culprit behind most spider veins, chronic venous insufficiency, has rather undesirable symptoms. Those patients might experience throbbing, aching, tingling, heaviness, itchiness, or muscle cramps. Patients with severe venous insufficiency deal with skin symptoms too, like poorly-healing ulcerations, discoloration, and dermatitis.
What Are the Causes of Spider Veins?
The basic reason behind spider veins is excess venous pressure. The pressure either builds within the vein walls, as with chronic venous insufficiency, or it’s imposed on the exterior vein walls, in the case of an injury. When the pressure is intravenous, it’s similar to a hose springing a leak. Rather than blood flowing seamlessly in one direction, some of the blood begins trickling out in different directions. Those leaky pathways are the spider veins you see beneath your skin.
How Do Our Vein Centers in Long Island Treat Spider Veins?
In the absence of disease, you might not need spider vein treatment from a health perspective. But our vein centers in Long Island often treat them with sclerotherapy to beautify your skin. Our vein doctors will determine if your spider veins represent something serious like blood clots or chronic venous insufficiency, which we treat with ultrasound-guided sclerosants or radiofrequency ablation.
What Are the Best Ways to Treat Spider Veins?
Treating spider veins is simple and safe, providing you choose a board certified vein doctor. No treatment should begin without a physical exam and evaluation of your symptoms. Some vein centers on Long Island offer cosmetic treatments, but those don’t address issues like chronic venous insufficiency. If you just treat the spider vein without treating the leaky valve, more veins will form. Our vein doctors in Long Island make sure your spider veins are really gone, by eliminating the actual problem.
Sclerotherapy
Often considered the treatment of choice for small spider veins, sclerotherapy uses either liquid, foam, or premixed foam irritants to destroy unhealthy veins. The medicine is injected into individual vessels and is one of the simplest solutions for spider veins.

Radiofrequency Ablation
Vein specialists use thermal energy to heat the spider vein’s walls, creating scar tissue that seals the vein shut. It’s a quick and gentle procedure, with a numbing solution on the skin and tumescent anesthesia surrounding the vein. It causes less pain and bruising than other types of ablation like EVLT.
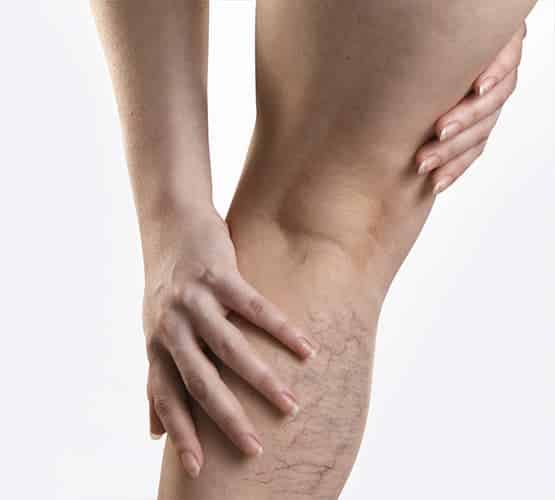
Endоvеnоuѕ Lаѕеr
Easier and safer than vein surgery, EVLT uses lasers to treat both venous insufficiency and spider veins. Since this procedure doesn’t require general anesthesia, patients don’t have to deal with the hospitalization and downtime associated with surgery.
Laser Therapy
Laser therapy at the skin’s surface is aimed solely at the visibility of spider veins. It’s most suited to the smallest veins and often is paired with sclerotherapy for flawless results. Lasers aren’t advised for those with sensitive skin, nor do they treat diseases like venous insufficiency.

Physical Activity
Like most health conditions, exercise is helpful for preventing spider veins. When you’re active, the muscles in your legs contract to push blood up toward the heart. If you already have spider veins, avoid sitting or standing for too long, and practice regular exercise. Aim for 30 minutes a day, and if you can, squeeze that exercise in between periods of sitting or standing to help your circulation. When you’re at rest, prop your legs above your heart level to reduce swelling and help blood travel in the right direction. Like compression stockings, exercise won’t get rid of the spider veins you have, but it will lessen symptoms and improve your circulation.
Compression Stockings
Support stockings might improve symptoms like swelling, since they apply steady pressure that helps your circulation. However, you need a proper fitting in order for them to work. The doctors at Long Island Vein Centers can measure you for the right pair. Keep in mind that compression stockings are only to manage symptoms and potentially prevent more spider veins from forming. They won’t eliminate existing spider veins or the disease that often causes them. Only a vein specialist can do that.